Natural Treatments for Iron Deficiency
Iron is an essential nutrient, but too much iron can lead to a number of chronic diseases, while too little iron can lead to many acute symptoms with the number one symptom being fatigue.
Many people suffer either from iron overload which generally speaking affects more men than women, or iron deficiency which generally speaking affects more women and children.
Finding the right balance is important, and because the symptoms of excess iron and iron deficiency can be similar, or related to many other health conditions, the only way to accurately know how your iron levels are is to do an iron studies blood test.
An iron studies blood test will measure iron, total iron binding capacity, transferrin, transferrin saturation and ferritin. We will talk more about these later and the optimal ranges for good health, the optimal range is different to the lab range that you will find on a blood test.
Before exploring natural treatments for iron deficiency, watch the video below to understand the most common and unusual symptoms, the tests that actually confirm iron deficiency, and why low iron is often missed or misunderstood.
Table Of Contents
Why do we need iron
- We require iron to produce red blood cells
- Hemoglobin which transports oxygen to the cells and tissues of the body
- Myoglobin which stores oxygen in the muscles to allow them to work optimally
- Energy production in the mitochondria
- DNA synthesis and cell division
- The production of enzymes which plays a role in the production of new cells, amino acids hormones and neurotransmitters
Iron is particularly important in childhood and pregnancy, as the developing baby depends solely on the mother’s supply from her diet, many common pregnancy multivitamins contain ferrous fumarate which is a poorly absorbed form of iron.
- Women are at a higher risk of iron deficiency because of the monthly menstrual cycle, this is more likely if the cycle is heavier or if the diet is low in iron. Menorrhagia is the medical term for excessively heavy periods, often caused by an estrogen imbalance and this is the biggest risk factor for low iron
- Children need the right amount of iron for growth and development, and of course energy production. Children with poor diets high in refined foods, or children who consume a lot of dairy are at risk of iron deficiency
- Elderly people often do not consume enough nutrient dense foods, have lower stomach acid to aid in the absorption of nutrients, this includes the cofactors for iron absorption like folate and B12 which are often low in elderly people
- Vegetarians and Vegans are at a higher risk of iron deficiency because they don’t consume heme iron from animal products which is the most easily absorbable form of iron. Vegetarian sources of iron are often high in phytic acid which reduces the absorption

- Elite athletes and weekend warriors are both at risk for iron deficiency if doing endurance sports, because of an increased demand for iron, and an increase in iron loss through sweat and even gastrointestinal bleeding.
- Gut infections can lead to an iron deficiency. Some bacteria use iron as a fuel source, which leads to low iron levels, but if you take iron supplements to address this it can make the digestive symptoms worse by promoting bacterial overgrowth.
- Gastrointestinal disorders like low stomach acid and IBS can lead to poor absorption of iron, while inflammatory bowel conditions like Ulcerative colitis and Crohn’s disease lead to iron loss through gastrointestinal bleeding
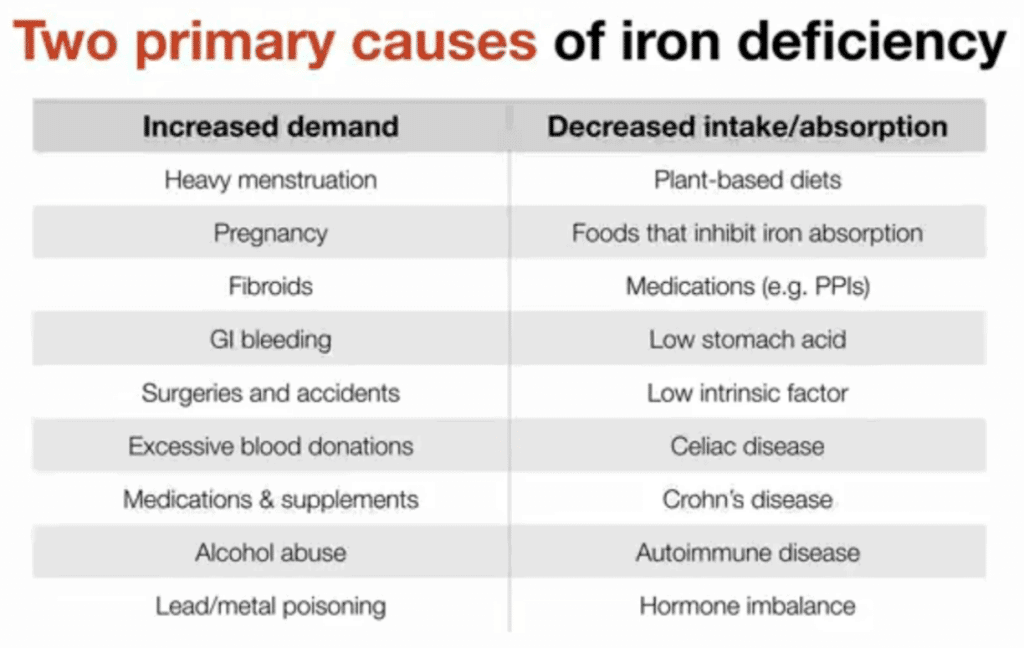
The two primary causes of iron deficiency are increased demand for iron, and a decreased intake or ability to absorb iron. The list of causes that come under each category means that a wide range of people are at risk of iron deficiency, the only way to know is to do an iron studies test, and not just think you need more iron and supplement “just in case”
Increased demand for iron
For women, the biggest cause of increased demand for iron is the menstrual cycle and pregnancy, especially during the reproductive years. As women approach menopause heavy periods and fibroids can cause iron deficiency anemia, and for the elderly a low intake of nutrient-dense foods, low stomach acid are the biggest cause of iron deficiency.
For men, the biggest cause of increased demand for iron is gastrointestinal bleeding, accidents and alcohol abuse. As men get older low intake of iron rich foods and gastrointestinal bleeding are the main causes of iron deficiency.
Decreased intake/ absorption
The most common reason for a decreased intake are people who are following a plant based diet, this is mainly because plants contain non-heme iron which is absorbed at less than half of animal-based heme iron. Plus many plants that are rich in iron also are high in phytic acid which also decreases the body’s ability to absorb iron. I have a lot of respect for people following a vegetarian/vegan diet for ethical or religious reasons and I would not want to discourage people from doing that, but it is important that they get an iron study test each year at a minimum to make sure they have optimal levels of iron.
Digestion problems and medications like proton pump inhibitors (use to treat reflux and one of the most overprescribed drugs) are a major cause of reduced iron absorption. In these cases addressing the cause of the iron deficiency is the first step in restoring optimal levels, rather than just taking a supplement.

How do we diagnose iron deficiency
An iron studies test is the best way to measure iron deficiency and while it gives you the blood level of iron, the two best markers of iron deficiency are Ferritin and Transferrin Saturation.
Ferritin is a protein synthesized by the body that is mainly used to store iron for future use, it is considered the most sensitive marker for iron deficiency. Ferritin is often the first marker to drop below the optimal range and can be an early indicator of inadequate iron levels.
Ferritin is also an acute-phase reactant that increases whenever there is inflammation in the body, so in some cases relying on ferritin as a marker for iron deficiency can be a bit misleading as the ferritin may be falsely elevated by inflammation. A good way to measure if the ferritin is elevated, or in the normal range because of inflammation is to also test HsCRP which is an inflammation marker and HbA1C which measures the glycation of red blood cells and is increased during times of inflammation.
The optimal reference range for ferritin
For women between 50-100
For men between 75-150
Transferrin saturation measures the amount of transferrin in red blood, transferrin is the main transport protein of iron. Optimal transferrin saturation levels are between 30-40% and this helps to transport the iron to all of the tissues, vital organs and bone marrow so normal metabolism, DNA synthesis and red blood cell production can take place.
Absorbed iron that is not needed for these purposes is stored as ferritin.
*** a high iron saturation % can be an indicator of iron overload.
Hemoglobin enables the red blood cells to transport oxygen through the bloodstream if hemoglobin levels are low as well as ferritin and transferrin saturation that means you have iron deficiency anemia. Low iron is not the only cause of anemia, and you can have low iron without anemia, this is another reason why testing is important to find out the cause of anemia.
B12 and Folate are cofactors for iron absorption and I would always recommend checking these levels when assessing your iron status.
Natural Treatments for iron deficiency
Diet is always the first treatment of choice when treating iron deficiency, along with addressing the underlying cause of why iron deficiency occurred in the first place.
Heme iron found in animal products is much better absorbed than non-heme iron which is the plant form of iron. The highest sources of heme iron are clams, liver, oysters, mussels and venison, these are all foods that are not commonly consumed in the standard diet. Lean red meat does contain iron but clams are 7X richer in iron than red meat and liver is 3X richer in iron than red meat.
I understand not everyone likes the taste of liver, but it can easily be mixed into stews or burger patties so that you would not even know that you are eating it. If your not a fan of liver then 2-3 servings of clams, oysters or mussels a week will really help to boost your iron levels.
Non Heme iron is found in plant-based foods, and the body’s ability to absorb non-heme iron is inhibited by phytic acid, oxalic acid, coffee, tea, and some fiber supplements. The best food sources of non-heme iron are spices, pumpkin seeds, sesame seeds, sun-dried tomatoes, natto, baked potatoes, and sunflower seeds.
Substances that reduce iron absorption
Calcium inhibits both heme and non-heme iron absorption if you have low iron I would not avoid calcium in food (reduce excess intake like drinking milk), but I would avoid calcium supplements. If you have osteoporosis and you have to supplement with calcium do it away from iron-rich foods or iron supplementation.
Eggs contain a compound called phosvitin that impairs absorption of iron. One boiled egg can reduce the absorption of iron in a meal by 28%, eggs, however, contain many beneficial nutrients and I would only limit eggs (or eat separately to iron-rich foods) if you are diagnosed with iron deficiency.
Oxalic Acid found in spinach, kale, beets, nuts, chocolate, and tea reduces the absorption of non-heme iron. So while kale and spinach have good amounts of iron, it is poorly absorbed because of the oxalates.
Polyphenols found in cocoa, coffee, black tea, herbs, and berries also inhibit non-heme iron from plant foods. Polyphenols also have many health benefits so I would not be avoiding these foods unless you are a vegetarian who is low in iron.
Phytic Acid found in soy protein, nuts, fiber, and some vegetables can reduce iron absorption by 50-60%
Zinc supplements, especially high doses of zinc over a long period of time can reduce iron absorption, if you need to take zinc supplements they are best taken away from other supplements, and away from food.
Substances that increase iron absorption
Vitamin C has been shown to increase both heme and non-heme iron absorption by up to 4 X
Beta-carotene significantly increases iron absorption, it can even cancel out the inhibitory effect of tannins and phytates in foods. Carrots are a good source of beta-carotene.
Betaine HCL is the acid that is present in the stomach and it helps with the breakdown of food and absorption of nutrients.
Alcohol increases iron absorption, especially red wine in moderation.
Treatment Summary
1/ The first step is to get tested, this can be done with your local doctor or contact Planet Naturopath
2/ Address underlying cause, this may include improving hormones to reduce heavy periods, improving digestion function or reviewing your medications.
3/ Improve your diet by increasing the iron-rich foods and decreasing foods that impair iron absorption
4/ Supplements to improve iron absorption include:
Thorne Research Iron bisglycinate for the best form of absorbable iron
Liposomal iron liquid easily absorbed and great for children or anyone who does not like tablets
Thorne Research Betaine HCL and Pepsin to improve digestion and iron absorption
Vitamin C can help the absorption of iron
These supplements are available from Amazon or www.iherb.com







